DR. ALAN TREVIÑO
OFTAMÓLOGO
SERVICES


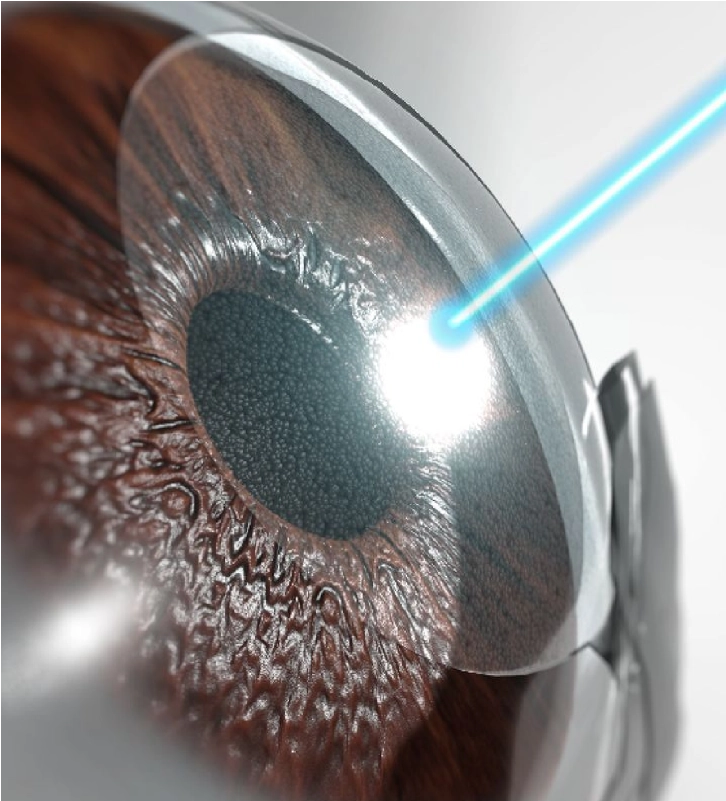
LASIK/FEMTOLASIK SURGERY
LASIK / Femto-LASIK SURGERY
Improve your vision! Reduce or eliminate dependence on glasses – no overnight stay.

RETINAL LASER
RETINAL LASER
State-of-the-art laser for the treatment of retinal holes and tears, diabetic retinopathy, and retinal vascular occlusion.
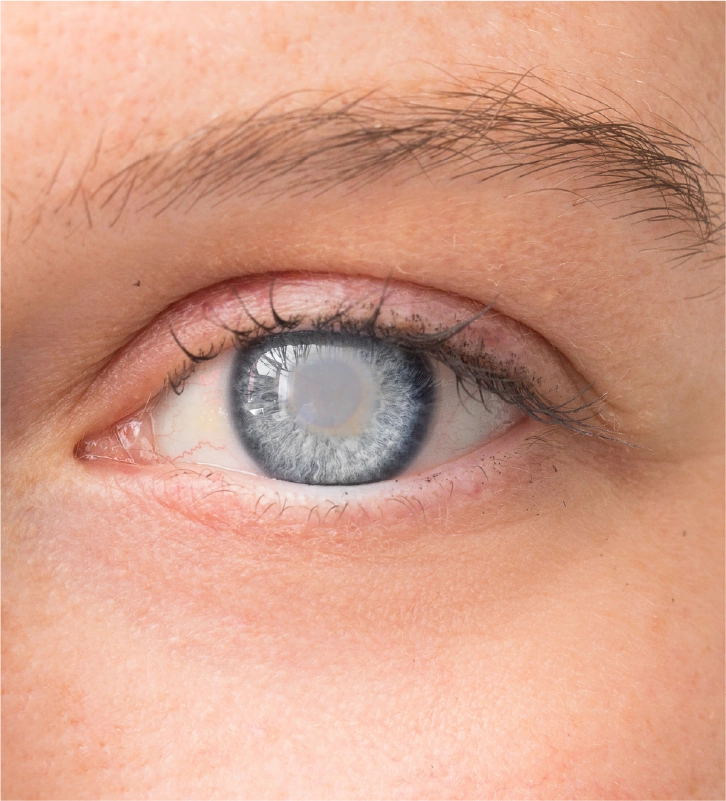
CATARACT SURGERY
CATARACT SURGERY
We use the latest technology to safely remove cataracts. No overnight stay.
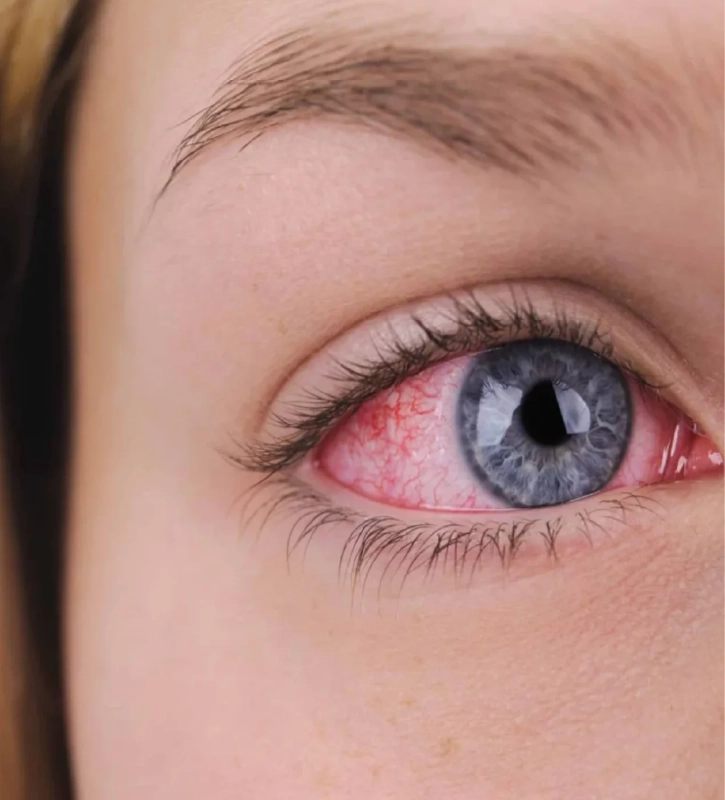
TREATMENT UVEITIS
TREATMENT UVEITIS
Treatment of inflammation or infection of the eye, whether or not associated with other systemic diseases.
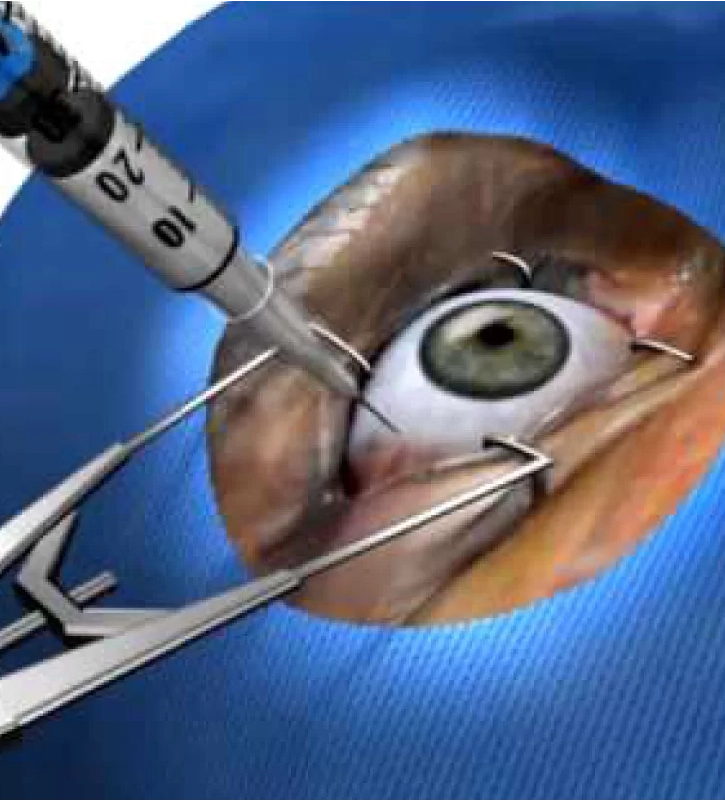
INTRAOCULAR INJECTIONS
INTRAOCULAR INJECTIONS
With anti-angiogenic and steroid drugs approved by FDA and COFEPRIS. No overnight stay.
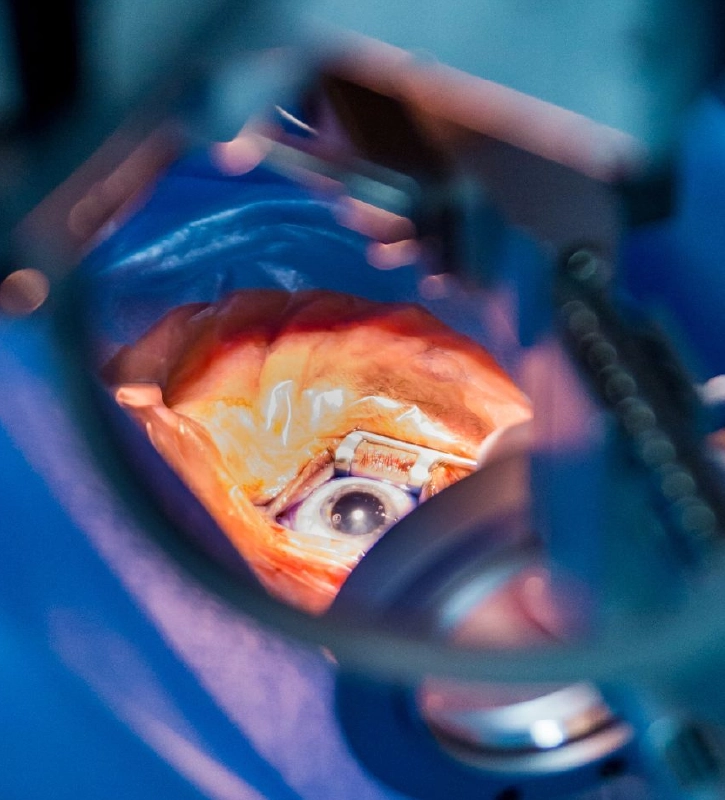
RETINAL SURGERY
RETINAL SURGERY
Surgery for retinal detachment, vitreous hemorrhage, diabetic retinopathy, and macular hole using the latest technology.
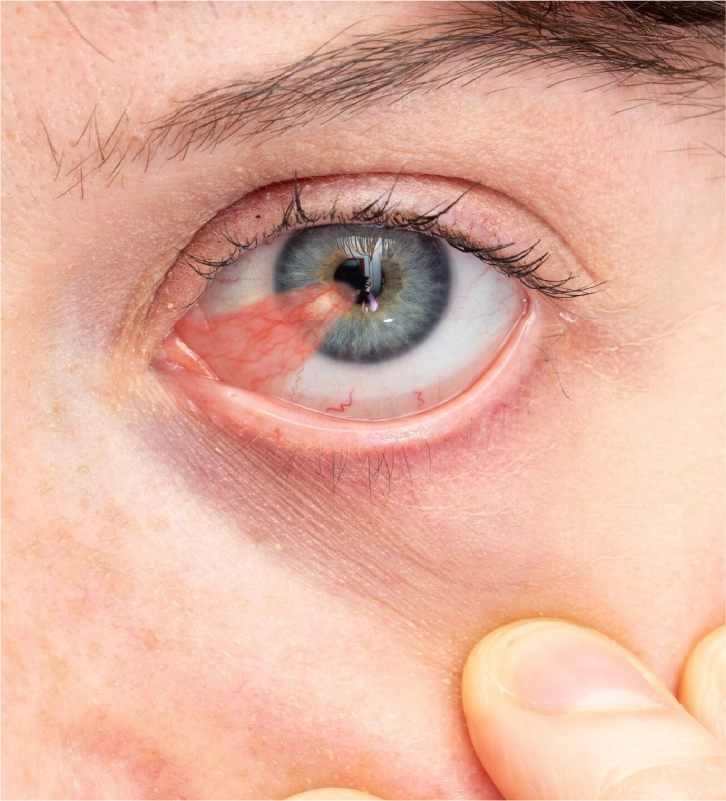
PTERYGIUM SURGERY
PTERYGIUM SURGERY
this is an outpatient, painless procedure performed under local anesthesia.
CROSS LINKING
CROSS LINKING
a surgical procedure that uses ultraviolet radiation together with a vitamin b2 solution to strengthen the cornea and prevent, delay, or reduce its progressive deformation.

EYEGLASS PRESCRIPTION
EYEGLASS PRESCRIPTION
a vision test that determines visual quality and how clearly a person can see objects at near, intermediate, or long distance.

CONTACT LENSES
CONTACT LENSES
they provide a full visual field without the interference of frames.

MYOPIA
MYOPIA
What is Myopia?
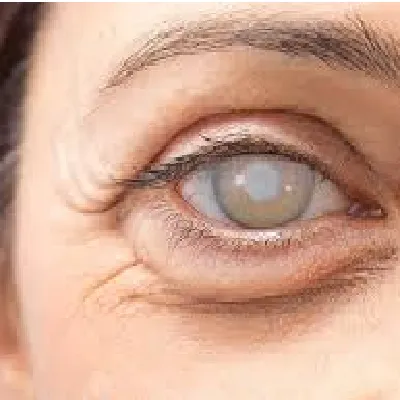
CATARACT
CATARACT
What is cataract?
EPIRETINAL MEMBRANE
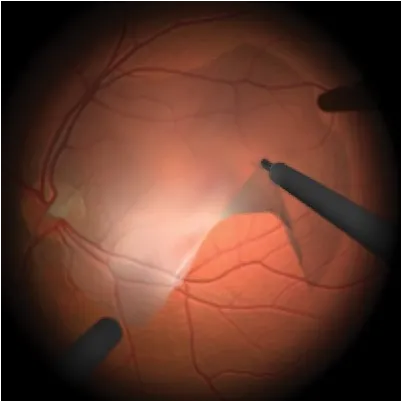
EPIRETINAL MEMBRANE
What is an epiretinal membrane?

HYPEROPIA
HYPEROPIA
What is hyperopia?
UVEITIS
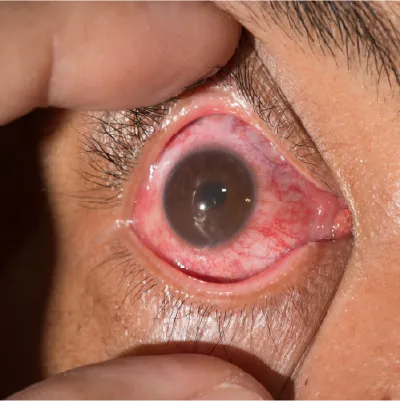
UVEITIS
What is Uveitis?
RETINAL DETACHMENT
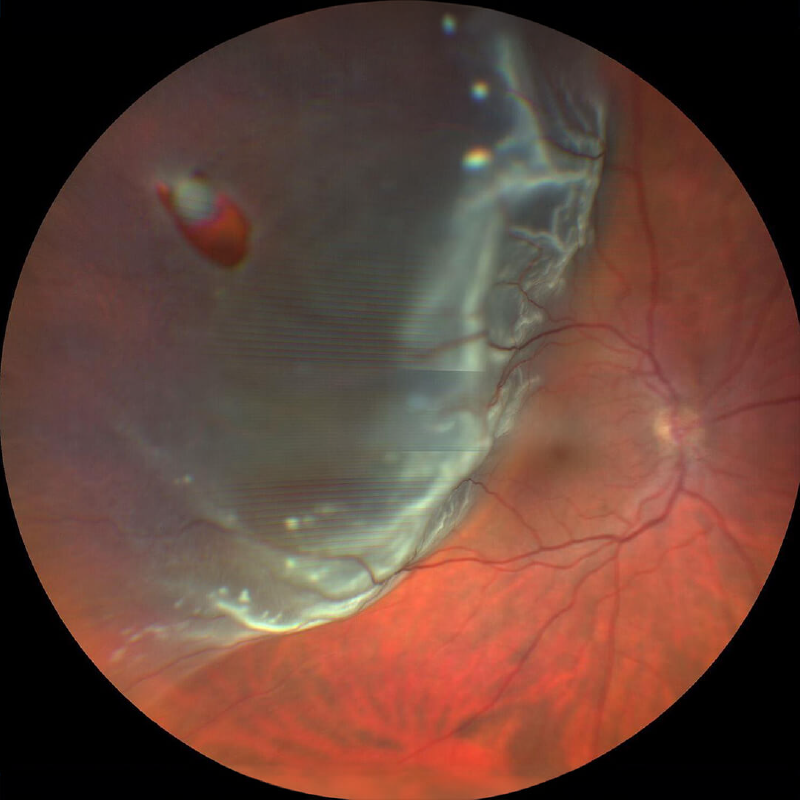
RETINAL DETACHMENT
What is retinal detachment?

ASTIGMATISM
ASTIGMATISM
What is astigmatism?
GLAUCOMA
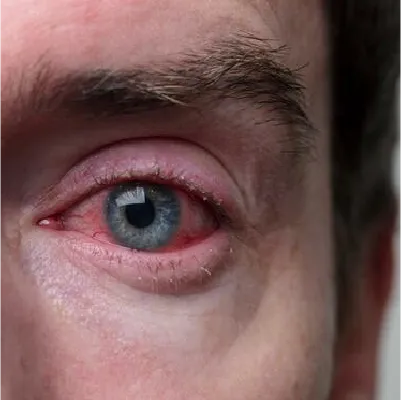
GLAUCOMA
What is Glaucoma?
DIABETIC RETINOPATHY
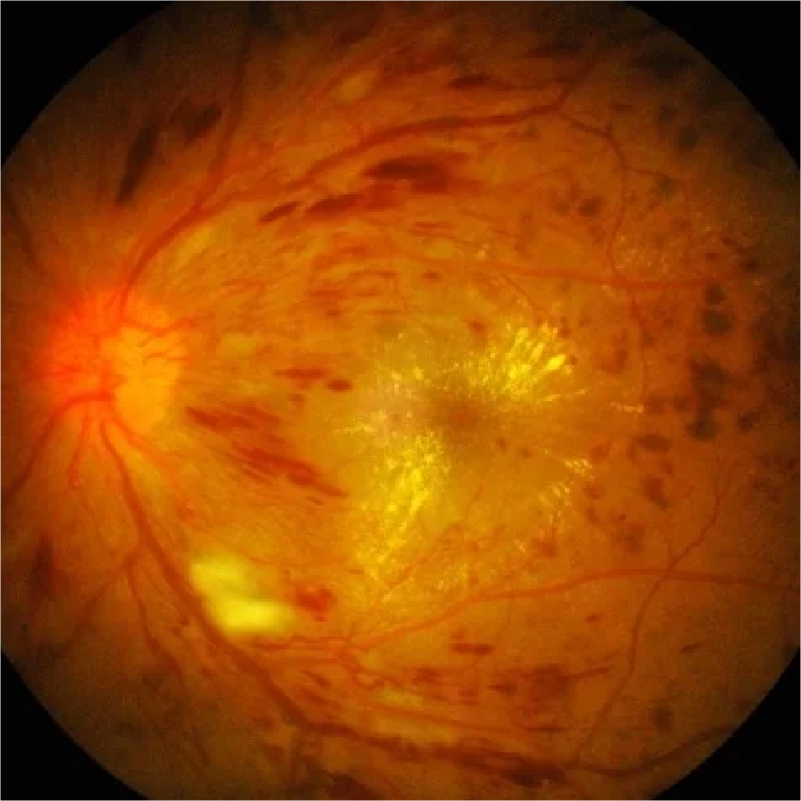
DIABETIC RETINOPATHY
What is retinopathy

PRESBYOPIA
PRESBYOPIA
What is presbyopia?

MACULAR HOLE
MACULAR HOLE
What is a macular hole?
AGE-RELATED MACULAR DEGENERATION
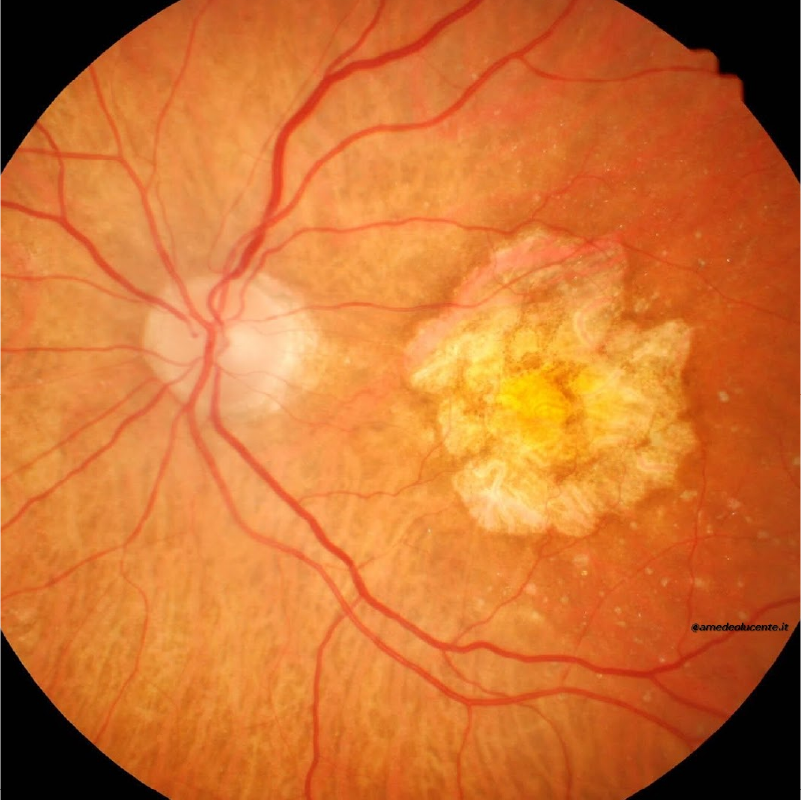
AGE-RELATED MACULAR DEGENERATION
What is age-related macular degeneration?

KERATOCONUS
KERATOCONUS
What is keratoconus?
DIABETIC MACULAR EDEMA
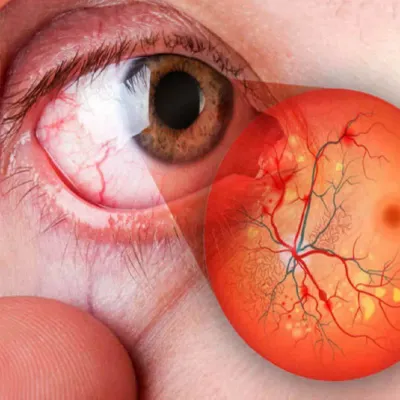
DIABETIC MACULAR EDEMA
What is diabetic macular edema?

Online consultation is a tool to identify potential vision problems or follow-up with our patients. The physician will decide the frequency of the presential visits based on the medical history and diagnosis.


VISIT US AT ANY OF OUR CLINICS
San Pedro Garza Garcia
Av. de la Industria 300 L-7 Col. Veredalta,
San Pedro Garza Garcia, Nuevo León, México.
Juárez City
Av. Hermanos Escobar 6637, Parque Industrial, Omega,
Juárez City, Chihuahua, México.
CONTACT US
FAQ
MYOPIA
What is myopia?
Myopia is a refractive error of the eye that causes blurred vision of distant objects, but clear vision of near objects.
Why does myopia occur?
It occurs when the eyeball is too long or the cornea or lens is too curved, causing light to focus in front of the retina instead of on it.
What causes myopia?
- Genetic factors: Myopia is usually inherited.
- Environmental factors: Spending a lot of time doing near activities, such as reading or using electronic devices, can increase the risk of developing myopia.
What discomfort does myopia cause?
- Blurred vision of distant objects.
- Squinting to see better.
- Getting closer to objects to see them.
- Headaches.
- Tired eyes.
How is myopia treated?
- Glasses or contact lenses: Correct nearsightedness by focusing light properly on the retina.
- Refractive surgery: Can correct nearsightedness by reshaping the cornea or lens.
- LASIK/FEMTOLASIK: Laser on the cornea.
- Phakic intraocular lens: Placement of an intraocular lens.
- Phacorefractive: Replacing the crystalline lens with an intraocular lens.
Can myopia be prevented?
Frequent breaks from near activities are recommended. Children need regular eye exams to detect and treat myopia early. Recently, eye drops, glasses with lenses made of special materials, and special contact lenses have been introduced that have been shown to slow the development of myopia in children.
HYPEROPIA
What is hyperopia?
Hyperopia, also known as farsightedness, is a refractive error of the eye that causes blurred vision of near objects, while distant objects are seen clearly. (when mild)
Why does hyperopia occur?
It occurs when the eyeball is too short or the cornea or lens is too flat, causing light to focus behind the retina instead of on it.
What causes hyperopia?
Genetic factors: Hyperopia may be inherited.
What discomfort does farsightedness cause?
- Blurred vision of close objects.
- Eye strain when reading or doing close work.
- Squinting to see better.
How is farsightedness treated?
- Eyeglasses or contact lenses: Correct farsightedness by focusing light properly on the retina.
- Refractive surgery: Can correct farsightedness by reshaping the cornea or lens.
- LASIK/FEMTOLASIK: Laser reshaping of the cornea.
- Phakorefractive: Replacement of the crystalline lens with an intraocular lens.
Can hyperopia be prevented?
- Frequent breaks from near activities are recommended.
- Children need regular eye exams to detect and treat farsightedness early.
ASTIGMATISM
What is astigmatism?
Astigmatism is a refractive error of the eye that causes blurred vision of both distant and near objects.
Why does astigmatism occur?
Astigmatism occurs when the cornea or lens has an irregular shape, similar to a football ball, rather than a smooth curved shape like a soccer ball. This causes light to focus on several points on the retina instead of just one, resulting in distorted vision.
What causes astigmatism?
- Genetic factors: Astigmatism is usually inherited.
- Environmental factors: Grinding your eyes can cause and worsen existing astigmatism.
What discomfort does astigmatism cause?
- Blurred vision of near and far objects.
- Eye fatigue.
- Squinting to see better.
- Difficulty seeing at night.
- Sensitivity to light
How is astigmatism treated?
- Glasses or contact lenses: Correct astigmatism by focusing light properly on the retina.
- Refractive surgery: Can permanently correct astigmatism by changing the shape of the cornea or lens.
- LASIK/FEMTOLASIK: Laser on the cornea.
- Phacorefractive: Replacement of the crystalline lens with a toric intraocular lens.
Can astigmatism be prevented?
- Frequent breaks from near activities are recommended.
- Children need to have regular eye exams to detect and treat astigmatism early.
PRESBYOPIA
What is presbyopia?
Presbyopia, also known as farsightedness, is an eye condition that affects most people over the age of 40. It is characterized by difficulty focusing on near objects, such as reading a book or using a cell phone.
Why does presbyopia occur?
Over time, the eye’s natural lens becomes less flexible and loses the ability to change shape to focus on near objects.
What causes presbyopia?
The main cause of presbyopia is the aging of the lens, the eye’s natural lens that helps focus light. Over time, the lens becomes less flexible and loses the ability to change shape to focus on near objects.
What discomfort does presbyopia cause?
- Difficulty focusing on near objects.
- Eye strain when reading or doing close work.
- Headaches.
- Squinting to see better.
- Moving text farther away to read.
- Need more light to read.
How is presbyopia treated?
- Glasses: Reading glasses are the most common way to correct presbyopia.
- Contact lenses: Multifocal or monovision contact lenses are an option for people who do not want to wear glasses.
- Refractive surgery: You can correct presbyopia by reshaping the cornea or lens.
- LASIK/FEMTOLASIK Monovision: Laser on the cornea.
- Phacorefractive: Replacement of the crystalline lens with a multifocal or extended focus intraocular lens.
Can presbyopia be prevented?
No.
Adults need to have regular eye examinations to detect and treat presbyopia early.
KERATOCONUS
What is keratoconus?
Keratoconus is a non-inflammatory, degenerative disease of the cornea, the transparent layer that covers the front of the eye. It is characterized by progressive thinning and protrusion of the cornea, which takes on a cone-like shape instead of its natural curved shape like a soccer ball.
Why does keratoconus occur?
Because of progressive thinning and protrusion of the cornea, which takes on a cone-like shape instead of its natural curved shape.
What causes keratoconus?
- Genetic factors: Keratoconus usually has a hereditary component.
- Environmental factors: Frequent eye rubbing, eye allergies, and certain diseases such as Down syndrome can increase the risk of developing keratoconus.
What discomfort does keratoconus cause?
- Blurred and distorted vision, especially at night.
- Progressive myopia and astigmatism.
- Sensitivity to bright light.
- Difficulty seeing at night.
- Double or multiple vision.
- Squinting to see better.
- Irregular astigmatism.
How is keratoconus diagnosed?
- Visual acuity.
- Refraction.
- Corneal topography: Measurement of the shape of the cornea.
- Optical coherence tomography (OCT): Measurement of corneal thickness.
How is keratoconus treated?
- Treatment of allergic conjunctivitis and avoidance of eye rubbing.
- Glasses or contact lenses: Correct blurred and distorted vision in mild cases. They do not slow the progression of the disease.
- Intracorneal rings: Acrylic rings inserted into the cornea to improve shape and vision.
- Corneal cross-linking: A procedure that strengthens the cornea using ultraviolet (UV) light and riboflavin. It slows the progression of the disease.
- Corneal transplantation: Replacement of the damaged cornea with a healthy one in severe cases.
Recommendations for keratoconus?
- People with keratoconus need to have regular eye examinations to monitor the progression of the disease.
- Eye rubbing should be avoided.
- If you have symptoms of keratoconus, please appoint me for appropriate treatment.
CATARACT
What is a cataract?
A cataract is a clouding of the crystalline lens, the eye’s natural lens that helps focus light. It is like the fogging of a window pane, causing vision to become blurred, cloudy, and less colorful.
Why does a cataract form?
The main cause is aging, but there are other causes such as trauma or eye injury, diabetes, glaucoma, prolonged exposure to sunlight, medications (steroids), and hereditary factors (genetic predisposition) that favor the development of cataracts.
What are the symptoms of cataracts?
Symptoms include blurred or cloudy vision, poor night vision, sensitivity to light, sunlight, or car lights, double vision, difficulty distinguishing contrasts and colors, and others.
How is a cataract removed?
Treatment consists of cataract surgery. This involves replacing the crystalline lens with an intraocular lens with a specific prescription for the affected eye. The intraocular lens may be monofocal (distance vision) or premium (distance and near vision).
How can I prevent cataracts?
Prevention consists of regular eye exams by an ophthalmologist starting at age 40 for early diagnosis. Proper control of metabolic diseases such as diabetes reduces the risk of developing cataracts. Wearing sunglasses with UV filters reduces the risk of developing cataracts. Avoid smoking, as smoking increases the risk of developing cataracts.
DIABETIC RETINOPATHY
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes that affects the blood vessels in the retina, the light-sensitive layer at the back of the eye. If left untreated, it can lead to blindness.
What causes diabetic retinopathy?
Diabetes can damage the small blood vessels in the retina, causing fluid and blood to leak. The number of years you have had diabetes and high blood glucose levels are the main risk factors for developing diabetic retinopathy.
Other factors, such as uncontrolled high blood pressure, high cholesterol and triglyceride levels, and smoking, can hasten the onset of diabetic retinopathy.
What symptoms does diabetic retinopathy cause?
- Blurred vision.
- Dark or floating spots in vision.
- Distorted vision.
- Severe visual loss or blindness.
How is diabetic retinopathy diagnosed?
A fundus exam, which requires dilating the pupils to see the entire retina in detail.
Other ancillary tests include macular OCT, which provides details of the area of increased vision or macula, and fluorescein angiography, which provides details of the retinal circulation.
What are the types of diabetic retinopathy?
Nonproliferative diabetic retinopathy (NPDR): This is the earliest stage of the disease. There is no growth of new blood vessels. However, if left untreated, it can progress to severe disease.
Proliferative diabetic retinopathy (PDR): This is the most advanced stage of the disease. It is characterized by the growth of new abnormal blood vessels in the retina. These blood vessels can become fragile and bleed, which can lead to vision loss.
How is diabetic retinopathy treated?
- Controlling diabetes: Keeping blood glucose levels under control is the best way to prevent diabetic retinopathy and slow its progression.
- Controlling blood pressure.
- Cholesterol control.
- Anti-angiogenic medications: Injections into the eye to treat the growth of new blood vessels.
- Laser photocoagulation: Laser treatment is used to reduce the oxygen demand of the retina and improve oxygenation of the retina.
- Vitrectomy: Surgery to remove the vitreous gel from the eye, remove traction membranes, and apply laser to the retina to control the disease.
What are the recommendations for a diabetic patient?
- It is important for people with diabetes to have regular eye exams to detect and treat diabetic retinopathy early.
- Diabetes, blood pressure, and cholesterol should be controlled.
- Smoking should be avoided.
- If you have symptoms of diabetic retinopathy, appoint me for appropriate treatment.
DIABETIC MACULAR EDEMA
What is diabetic macular edema?
Diabetic macular edema (DME) is a complication of diabetes that affects the macula, the central part of the retina responsible for central and detailed vision. It occurs when fluid leaks from damaged blood vessels in the retina and accumulates in the macula.
What causes diabetic macular edema?
High blood sugar: Diabetes can damage the small blood vessels in the retina, causing leakage and fluid accumulation.
High blood pressure and high cholesterol increase the risk of DME.
What symptoms does diabetic macular edema cause?
- Blurred vision.
- Distorted vision.
- Difficulty reading
- Difficulty seeing at night.
- Sensitivity to light.
How is diabetic macular edema diagnosed?
A fundus exam requires dilating the pupils to see the macula and the entire retina in detail.
Other ancillary tests, such as macular OCT, provide details of the macula that are key to diagnosis and patient follow-up.
How is diabetic macular edema treated?
- Diabetes control: Keeping blood glucose levels under control is the best way to prevent DME and slow its progression. Control blood pressure and cholesterol.
- Antiangiogenic drugs: Injections into the eye used to prevent fluid leakage from damaged blood vessels.
- Focal laser photocoagulation: Laser treatment is used to seal leaking blood vessels.
- Vitreoretinal surgery: Surgery to remove the vitreous gel from the eye and relieve any traction areas that cause macular edema with a tractional component.
What are the recommendations for a diabetic patient?
- People with diabetes need to have regular eye exams to detect and treat DME early.
- Diabetes, blood pressure, and cholesterol should be monitored.
- If you have symptoms of DME, consult me for appropriate treatment.
AGE-RELATED MACULAR DEGENERATION
What is Age-Related Macular Degeneration?
Age-related macular degeneration (AMD) is an eye disease that affects the macula, the central part of the retina responsible for central and detailed vision. It is the leading cause of legal blindness in people over the age of 60.
What are the types of AMD?
- Dry AMD: This is the most common form of the disease. It is characterized by thinning and loss of cells in the macula.
- Wet AMD: This is a less common but more severe form of the disease. It is characterized by the growth of abnormal blood vessels under the macula that can leak blood and fluid.
What causes AMD?
- Age: The most important risk factor for AMD is age.
- Genetics: AMD can be inherited.
- Smoking: Smoking cigarettes increases the risk of developing AMD.
- Obesity: Abdominal obesity may increase the risk of developing AMD.
What symptoms does AMD cause?
- Blurred vision in the center of the field of vision.
- Difficulty reading or doing near activities.
- Distorted vision.
- Decreased color perception.
- Sensitivity to light.
How is AMD diagnosed?
- Visual acuity.
- Fundus examination.
- Optical coherence tomography (OCT): Measurement of retinal thickness; key to diagnosis and patient follow-up.
- Fluorescein angiography: Test that uses a dye to evaluate the retina.
How is AMD treated?
- Control risk factors: Stop smoking and control body weight.
- Antioxidants and vitamins: It has been shown that some supplements, such as lutein and zeaxanthin, can reduce the risk of progression of AMD.
- Intravitreal injections: Injections into the eye of anti-angiogenic drugs that are used to stop leakage and prevent new blood vessel growth in wet AMD.
What are the recommendations for preventing AMD?
- People over the age of 50 need to have regular eye exams to detect and treat AMD early.
- Body weight should be controlled and smoking should be stopped.
- If you have family members with AMD or symptoms of AMD, consult with me to assess your case.
MACULAR HOLE
What is a macular hole?
A macular hole is a small circular opening that forms in the macula, the central part of the retina that is responsible for central and detailed vision. It occurs when a small area of the macula thins and ruptures.
What causes a macular hole?
- Aging: The most common cause of a macular hole is aging. As we age, the vitreous (the clear jelly-like fluid that fills the eye) shrinks and separates from the retina. In some cases, the vitreous can pull on the retina and cause a macular hole.
- Eye trauma: A blow or injury to the eye can cause a macular hole.
- Myopia: People with myopia have an increased risk of developing a macular hole.
What discomfort does a macular hole cause?
- Blurred vision in the center of the visual field.
- Distorted vision.
- Perception of a dark spot in the center of vision.
- Difficulty reading or performing near activities.
How is a macular hole diagnosed?
- Visual acuity.
- Examination of the fundus.
- Optical coherence tomography (OCT): Key to diagnosis, and measurement of the macular hole.
How is a macular hole treated?
- Observation: Small macular holes may not require treatment.
- Vitrectomy: Surgery to remove the vitreous and relax the edges of the macular hole.
EPIRETINAL MEMBRANE
What is an epiretinal membrane?
An epiretinal membrane (ERM) is a thin layer of scar tissue that forms on the surface of the retina, the light-sensitive layer at the back of the eye. It affects the macula, the central area of the retina responsible for central and detailed vision.
What causes epiretinal membranes?
In most cases it is idiopathic or unknown. In some other cases, it can be identified as secondary to previous inflammation, diabetes mellitus, retinal holes, etc.
What symptoms does an epiretinal membrane cause?
- Blurred vision.
- Distorted vision.
- Difficulty reading or doing near activities.
- Perception of a spot or wrinkle in the field of vision.
How is an epiretinal membrane diagnosed?
- Visual acuity.
- Fundus examination.
- Optical coherence tomography (OCT): To assess the anatomy and thickness of the macula. Key for the diagnosis and follow-up.
How is an epiretinal membrane treated?
- Observation: Asymptomatic or mildly symptomatic ERMs may not require treatment.
- Vitrectomy with membrane peeling: Surgery to remove the vitreous and remove the epiretinal membrane from the surface of the retina.
What are some recommendations for patients with ERM?
People with symptoms of ERM need to consult an ophthalmologist for appropriate treatment.
RETINAL DETACHMENT
What is a retinal detachment?
A retinal detachment is a serious eye condition in which the retina, the light-sensitive layer at the back of the eye, separates from the underlying layer called the retinal pigment epithelium. When this happens, the retina cannot function properly and vision loss occurs.
What causes a retinal detachment?
- Retinal tear: A tear or hole in the retina can allow fluid to seep under the retina and separate it from the pigment epithelium.
- Eye trauma: A blow or injury to the eye can cause retinal detachment.
- Eye disease: Diabetic retinopathy may increase the risk of retinal detachment.
- Eye surgery: Rarely, a retinal detachment may occur after eye surgery.
What are the symptoms of retinal detachment?
- Flashes of light: Flashes of light in the visual field, especially in peripheral vision, maybe a sign of a retinal tear, which may precede a retinal detachment.
- Floaters: Floaters are small spots or specks that float in the visual field. If they appear suddenly or increase in number, they may be a sign of a retinal tear.
- Blurred vision: Blurred vision, especially in peripheral vision, may be a sign of early retinal detachment.
- Curtain or veil in the visual field: The perception of a curtain or veil falling may be a sign of retinal detachment.
How is retinal detachment diagnosed?
- Visual acuity.
- Fundus examination.
How is a retinal detachment treated?
- Laser photocoagulation: Used to seal retinal tears and prevent retinal detachment.
- Cryotherapy: Used to freeze and seal retinal tears.
- Surgery: There are different types of surgery to repair retinal detachment, such as placement of a cerclage, pneumoretinopexy, or vitrectomy.
What are some recommendations for patients with retinal detachment?
People with symptoms of retinal detachment must visit an ophthalmologist immediately.
GLAUCOMA
What is glaucoma?
Glaucoma is a group of eye diseases that damage the optic nerve, which is responsible for sending the images we see to the brain. This damage can cause vision loss and, if left untreated, can lead to blindness.
What are the risk factors for glaucoma?
- High intraocular pressure: This is the main risk factor for glaucoma.
- Age: The risk of glaucoma increases with age.
- Race: African Americans and Hispanics have a higher risk of developing glaucoma.
- Family history: Having a family member with glaucoma increases the risk for the disease.
- Diseases: Some diseases, such as diabetes, high blood pressure, and sleep apnea, can increase the risk of glaucoma.
What symptoms does glaucoma cause?
- Loss of peripheral vision (side vision).
- Blurred vision.
- Eye pain.
- Nausea and vomiting.
- Redness of the eyes.
- Sensitivity to light.
How is glaucoma diagnosed?
- Visual acuity.
- Intraocular pressure measurement.
- Pupil dilation.
- Examination of the fundus.
- Optical coherence tomography (OCT): Measurement of the retinal nerve fiber layer.
- Campimetry: Determination of the visual field.
How is glaucoma treated?
Glaucoma treatment aims to reduce intraocular pressure and prevent damage to the optic nerve. It may include:
- Medications: drops or pills to reduce intraocular pressure.
- Laser: Selective laser trabeculoplasty (SLT) or laser peripheral iridotomy (YAG) to improve drainage of the aqueous humor.
- Surgery: Trabeculectomy or valve implantation to create a new aqueous drainage pathway.
What are some recommendations for patients with glaucoma?
People with risk factors need to have regular eye exams to detect the disease early.
If you have symptoms of glaucoma or a family history, appoint me for appropriate treatment.
UVEITIS
What is uveitis?
Uveitis is an inflammation of the uvea, the middle layer of the eye. The uvea contains many blood vessels that nourish the iris, ciliary body, and choroid.
Types of uveitis:
- Anterior: Affects the iris and ciliary body.
- Intermediate: Affects the pars plana, which is the posterior part of the ciliary body.
- Posterior: Affects the choroid.
- Panuveitis: Affects the uvea in all 3 areas equally.
Causes:
- Autoimmune diseases: Uveitis can be caused by autoimmune diseases such as ankylosing spondylitis, psoriatic arthritis, Crohn’s disease, and sarcoidosis.
- Infections: Some infections, such as toxoplasmosis, tuberculosis, and syphilis, can cause uveitis.
- Trauma: A blow or injury to the eye can cause uveitis.
- Other: Some types of cancer, exposure to toxins, and medications can cause uveitis.
Symptoms:
- Eye pain.
- Redness of the eyes.
- Sensitivity to light.
- Blurred vision.
- Loss of vision.
Diagnosis:
Is made by a complete eye examination including:
- Visual acuity.
- Fundus examination
- In some types of uveitis, tests may be needed to determine the cause of the uveitis or to rule out systemic disease.
Treatment:
Depends on the cause and severity of the inflammation. It may include:
- Anti-inflammatory medications: Corticosteroid drops, tablets, or injections.
- Immunosuppressive medications: Used to control inflammation in chronic and severe cases.
- Antibiotics or antivirals: Used to treat infections that cause uveitis.
- Surgery: Surgery may be performed to treat complications of uveitis.
LASIK / FEMTOLASIK
I want to have LASIK/FEMTOLASIK surgery. What should I do?
- Schedule an appointment for a complete evaluation of your eyes and determine your lens prescription.
- A cornea study is performed to determine if the patient is a candidate for surgery.
- If the patient is a candidate, the surgery can be performed that same day. The surgery is performed on an outpatient basis. The surgery takes 10-15 minutes for both eyes, the type of anesthesia is in drops. At the end, protective lenses will be placed.
- The patient comes for evaluation the next day after surgery.
After surgery, when will I be able to see clearly?
On the day of surgery, vision will be blurred, you may feel a foreign body sensation and tearing. The following day, vision will be close to 100% and discomfort will be minimal.
Who are candidates for LASIK/FEMTOLASIK surgery?
Most people are candidates for surgery. Patients with myopia, hyperopia, or astigmatism may be candidates. For patients not candidates for LASIK/FEMTOLASIK, techniques such as PRK or phakic lens implantation may be explored.
Indications after LASIK/FEMTOLASIK surgery
The recovery time is short; the day after surgery, vision is nearly 100%, and it is likely to be able to work. Eye rubbing should be avoided.
I am a foreigner. What is the procedure I have to follow to have my surgery?
It takes at least 2 days. The evaluation and surgery can be done on the same day. It is important to have an assessment the day after the surgery and then you can go home.
Can I have the surgery if I wear contact lenses?
Of course, you can. However, it is important to stop wearing soft contact lenses (at least 1 week) and rigid gas permeable contact lenses (2 weeks) before the exam and surgery.
How long will the effects of LASIK/FEMTOLASIK surgery last?
Distance vision is preserved until age 55-70, when cataracts appear, and near vision is altered at 40-45 years, as it is in all people due to presbyopia. In some cases, lens prescription may appear again if the eye has changed its curvature or size after surgery.
How should I take care of myself after LASIK/FEMTOLASIK surgery?
The most important thing is to avoid rubbing your eyes. It is important to avoid water or soap when bathing. The patient will use the prescribed eye drops to control inflammation and prevent infection.
When can I go back to work?
2 days after surgery.
Is the surgery painful?
The surgery is done under topical anesthesia (eye drops) and it’s painless.
How long does the surgery take?
Approximately 10-15 minutes for both eyes.
Am I candidate for LASIK/FEMTOLASIK?
We can find out by performing a complete ophthalmic examination and with a corneal topography. In this study, we will see the thickness and curvature of the cornea, and we will be able to exclude corneal diseases.
CROSS LINKING
- What is corneal crosslinking?
Corneal crosslinking, also known as corneal interlinking or corneal bonding, is a minimally invasive outpatient procedure used to treat keratoconus.
- How does corneal crosslinking work?
It works by strengthening the structure of the cornea. This is accomplished by applying a riboflavin (vitamin B2) solution to the surface of the eye, followed by exposure to ultraviolet A (UVA) radiation. The UVA light activates riboflavin, which generates cross-links between the collagen fibers of the cornea. These cross-links make the cornea more rigid and resistant to bulging.
- When is crosslinking recommended?
It is recommended primarily for patients with progressive keratoconus.
- What are the benefits of corneal crosslinking?
- Stopping or slowing down the progression of keratoconus.
- Prevention of corneal scarring
- Preventing the need for corneal transplantation.
PTERYGIUM SURGERY
- How is pterygium surgery performed?
It is performed under local anesthesia. I use a microscope to carefully remove the pterygium. In addition, a conjunctival graft from another part of the eye (graft) is used to cover the area where the pterygium was removed.
- What should I expect after pterygium surgery?
Recovery after pterygium surgery is usually quick. Most people can return to their normal activities the next day.
- Can a pterygium recur?
A preoperative evaluation to exclude conjunctival inflammatory diseases is key to avoid recurrences. Surgery with conjunctival graft has the lowest recurrence rate, about 5% of cases.
- What are the goals of pterygium surgery?
- Improve vision.
- Decrease astigmatism.
- Symptom relief.
- Aesthetic improvement.
- Double vision relief in very advanced cases.
CATARACT SURGERY
- What is cataract surgery?
It is a procedure in which the natural lens of the eye is removed and replaced with an artificial lens.
- How is cataract surgery performed?
It is performed through a small incision in the eye and the phacoemulsification technique is used to break up the cataract and remove it.
- Is cataract surgery painful?
No, cataract surgery is performed under local anesthesia and it is painless.
- How long does cataract surgery take?
It usually takes 10 to 15 minutes.
- When can I return to work after cataract surgery?
Most people can return to work and normal activities within a few days after cataract surgery.
- How long does it take to recover from cataract surgery?
Recovery from cataract surgery varies from person to person; it usually takes 1 to 2 weeks.
- Is cataract surgery safe?
Yes, cataract surgery is a very safe and effective procedure.
- Do I need to wear glasses after cataract surgery?
It depends on the intraocular lens that was placed in the eye during surgery. Premium lenses allow distance and near vision without glasses, while monofocal may require glasses for near vision.
- Can I have cataract surgery on both eyes on the same day?
It is generally not recommended for both eyes at the same time. In most cases, the surgery is performed on one eye and then on the other eye at least 1 week later.
RETINAL LASER
What is a retinal laser?
Retinal laser, also known as retinal laser photocoagulation, is a medical procedure that uses a highly focused beam of laser light to treat a variety of eye conditions affecting the retina.
How does the retinal laser work?
The retinal laser works by cauterizing retinal tissue. The laser creates small controlled burns in the retina, which helps oxygenate the retina, seal abnormal blood vessels, and stop the growth of new tissue. The burned area increases the adhesion of the retina.
In what cases is retinal laser recommended?
The retinal laser is recommended to treat a variety of eye conditions, including:
- Diabetic retinopathy: A complication of diabetes that causes damage to the blood vessels of the retina. Laser can help prevent blindness by stopping the growth of abnormal new blood vessels.
- Retinal venous and arterial occlusions: These are blockages in the veins or arteries that supply the retina. Laser can help prevent vision loss by preventing the growth of abnormal new blood vessels.
- Retinal detachment: This occurs when the retina separates from the back of the eye. The retinal laser can help to keep the retina back in place and it is applied during surgery. Preventive lasers may be done around retinal breaks to reduce the risk of retinal detachment.
What are the benefits of retinal lasers?
The benefits of retinal laser include:
- Prevention of vision loss
- Stabilization of eye disease
- Reducing the risk of complications
What should I expect after the retinal laser?
Recovery after retinal laser is fast. Most people can return to their normal activities the next day.
INTRAOCULAR INJECTIONS
What are intravitreal injections?
Intravitreal injections are a medical procedure that consists of injecting a drug directly into the vitreous cavity inside of the eye.
What are intravitreal injections used for?
Intravitreal injections are used to treat a variety of eye diseases such as:
- Wet age-related macular degeneration (AMD).
- Diabetic macular edema.
- Retinal venous or arterial occlusion.
- Choroidal neovascularization.
- Uveitis.
RETINAL SURGERY
There are different techniques to perform retinal surgery. Among the different techniques, there is an external approach with cerclage and an internal approach with vitrectomy. Some of the diseases to be treated are:
- Diabetic retinopathy
- Macular hole
- Epiretinal membrane
- Retinal Detachment
GLAUCOMA
There are different surgeries and procedures for glaucoma control, such as filtering surgery, valve implantation, YAG laser peripheral iridotomy, and cataract surgery, among others.
CONTACT LENSES
- SofT
- Rigid Gas Permeable
- Scleral


